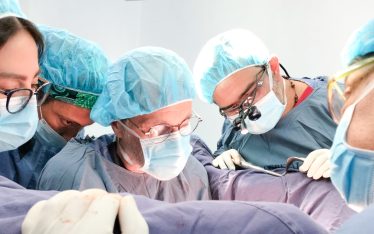
We were very honored to invite Dr Sanjay Pandey for our next interview. Doctor Pandey is head of Andrology and Reconstructive Urology in Kokilaben Dhirubhai Ambani Hospital in Mumbai, India.
Dr Pandey prepared a presentation about Gender Reassignment Surgery that he commented during the live interview. The PowerPoint presentation can be found in the replay (from minute 8:30). The doctor also told us about his experience, surgery procedures and answered your questions.
Watch the replay of his interview here!
Can you tell us about yourself and your activity?
I started as a consultant urologist at Kokilaben Dhirubhai Ambani Hospital in Mumbai, India. I am part of the team of transplant and reconstructive urology and I co-ordinate the Gender Reassignment Team comprising Endocrinologists, Psychiatrists, Gynecologists, Plastic Surgeons and Voice-Speech Therapists. It is a multidisciplinary hospital.
In 2008, I began to be really involved in reconstructive urology. I joined a fellowship in Gender Reassignment Surgery in Serbia, with Dr. Miroslav Djordjevic who was a great teacher for me. As a team, we performed FTM and MTF surgeries.
What king of gender reassignment surgeries do you perform?
I perform metoidioplasties, phalloplasties and vaginoplasties.
Metoidioplasty might not be a step towards phalloplasty, but the individuals have decided to undergo a change months / years later but they can get a phalloplasty after a metoidioplasty.
Can you tell us about metoidioplasty?
It is a single stage surgery. The clitoris is expected to enlarge with the take of hormones. We are converting the entrapped clitoris into a small phallus by stretching it. The only visible part of the clitoris is the tip of the glans. We have achieved 4 to 7 cm (depending on the hormones enlargement). Then we can do a urethral prolongation. Even if the metoidioplasty is not long enough to have intercourse with penetration, it is possible to void standing.
Could you tell us about your techniques for the phalloplasty?
I learned in Serbia the dorsal flap technique. But when I came back to India, I noticed our patients had different needs. They are not as tall, so the size of the phalloplasty would not have been appropriate with this technique. Compared to what is god given, you accept it as a part of the body. Something that the surgeon gives you will look too small or too big because it is not exactly matching your expectation. It is important to have realistic expectations.
Today we perform pedical flaps at Kokilaben Hospital, which is ALT flap that we do in different stages. At the first stage, we create the phalloplasty. Patients stay to the hospital 7 to 10 days, and they can go home. The organ matures, the patient and the partner accept the organ and get a partial sensation to it, and they come back for the next stage which can be the urethroplasty or the implantation of the malleable prosthesis.
The scrotoplasty, when do you do it?
It is possible to do it at the last moment, when the journey is almost over. We can put an expander in advance. It allows to get enough skin and help to put then a testicular implant later on. The scrotoplasty can be done from the labia, and little later on, patient can ask for a urethral lengthening. But it is the most challenging part of the all thing.
Does it mean that you automatically perform urethral lengthening? Or is it according to patient’s expectation?
Every individual is different and decides if they want UL or not. Sometimes patients come to us after 6 months or 3 years post phalloplasty, it depends. To me, urethroplasty can be done at the stage when the neo-phallus is healed and has a size from 12 cm to 15 cm (no longer than that though).
We create the urethra by a tunnel approach, it is about creating a pedicled flap from the perineum. For anybody undergoing hysterectomy, I request that the vagina is not disturbed. It is a very important resource organ for me, to be able to create flaps for a continuity of the urethra.
Many patients would say they want only a phallus. But the majority of them want a urethroplasty between 6 months and 2 years for sure. Sometimes the implant has come before urethroplasty, but more frequently after. We are very careful about where to implant the urethra, and where to implant the prosthesis. The prosthesis goes dorsal, the urethra goes ventral.
Is the finality of the phalloplasty to have an implant?
80 to 95% of patients will look at a final completion in a phalloplasty. It means there are looking at the sensate functional organ created by the reconstructive urologist.
When we look at final completion, a majority of them would like an implant for coitus.
For you, what is the advantage with implants specifically designed for the phalloplasty?
For me, the fixation plate is really important. This makes the difference compared to other existing cismen implants. ZSI implants are specially structured to fit in a phalloplasty, and results are very promising. So, we hope to be able to use them very soon!
Could you talk about MTF surgeries?
MTF is close to my heart because it is the first surgery I did. One technique we do is the penoscrotal inversion. This technique has to do with the length and the depth of the organ that we create from the organ which is available. It is all about removal of the corpus bodies and the testis to create the clitoris, which is a sensitive organ. The vaginoplasty has an aesthetic function (with the major labia and the minor labia), but it is also functional and allows the patient to have sensations. Since last year, we took the lead forward in the subject of vaginoplasty in terms of being able to do robotic assisted vaginoplasty. It is important to understand that there are females born without vagina such as men born without a phallus.
Do you receive sometimes foreign patients who already have a phalloplasty or a metoidioplasty, and want a revision or an implantation of device, or a urethra lengthening?
Yes, we receive patients from Asia, Africa, and also Europe and a few Americans. From the last 10 years, we have patients coming from almost all over the world.
Patients come in requesting a change, for revision or to begin with a gender reassignment surgery.
My colleagues in India have taken this into a very high level already. I am just representing them. The more we do, the more we will see and so that we can help our patients to have realistic expectations. We are making them understand that it is a journey where every life matter and we want to improve it.
If a patient had hormones blockers at early age, the phallus would not be long enough, there is not enough skin to have the penile inversion, what do you do in this case?
Sometimes we can use the scrotum, which would have been laser depilated completely. It is all about stretching as much as possible.
We need to bring downs the expectations to a proper level of realistic expectations. But it is important to explain to the patients what we are capable of.
Is it possible to have surgery before the patient turns 18?
It would be against the law and the science. We are operating people from 21, 22 years old. But we also have patients in their late 50s. It is very important to keep in mind that it is an irreversible surgery. For very young people, we recommend a continuous psychological support. Moving forward in the journey, as they reach maturity turning 18 to 21, we talk with the family, the peers, the workplace to make sure they are psychologically stable before we look into something that would be irreversible.
What are the medical challenges if we are planning surgery in the early 40s?
At this age, it means that you had time to understand yourself and you are ready to move to the next step of surgery. If there is no medical contra indication, patients can begin the process.
We get more 20 and early 30s. In general, they have a more comfortable financial situation (in India, people are not covered for reassignment surgeries). It is not only the age. It depends if people are starting their journey and just began to take hormones, in that case we will wait for them to be at a more advanced stage of their transition.
Could you show how the scars look like?
I am not able to show any pictures. It is just about making the scar as invisible as we can. The scar can be hidden with clothes. And as time will pass by, the scar will be less visible. It depends on the phalloplasty technique, it is never scarless, but we try to do it at the minimum.
What do you think will be the next big thing for FTM surgeries?
We are all looking to innovate. Improving our own results, improving our team work, using ZSI implants which are the most innovative implants for both FTM and MTF surgeries with now the vaginal stent. It helps us to innovate. This is the kind of implant that could help to give more stretch to the neovagina. We are looking at life savings, life changing, life extending therapy on these patients who deserve to get this.
What do you think about the inflatable ZSI 475 FTM implant?
It seems to me that ZSI implant is a wonderful implant, specially structured to fit in a phalloplasty, but my colleagues have more experience of it. So far it is early to speak about how it will be in 10 years. But when we look at results with cis men implants, results are very promising. So, we hope to be able to use them very soon!
What is the resting period post-surgery that you recommend for patients coming from abroad?
For patients coming from other cities around, for the 1st stage of FTM, we recommend to stay 7 to 10 days (7 days is a minimum so that they are able to walk). MTF we recommend 9 to 13 days (depending on their own comfort). I don’t discharge people as early as they do in Europe because they don’t live next door. These are complex surgeries and have not been completed in India to such a high level. People do rest back home. Then it takes a few more weeks before they can go back to work, before they can run…
If you had to choose between esthetic or functionality, what would be your priority/recommendation?
From an ethical point of view, no GRS surgeon wants to do huge numbers… They only want to do their best to respond to the patient’s demand. So, to me it is a balance between esthetics, functionality, capability, and ethics.
Does your hospital conduct any awareness campaign about trans people’s care specifically?
Some of our patients have lost their job and their home because they don’t have any support of their peers or family anymore. So, the work of NGOs, organizations and associations on that level is really important to take care of these people. We have operated people who are now role models. The country moves forward, the support is always there.
I am very sensible to the quality of life and the need of our patients, especially as we are talking about patients who don’t have any disease. Our hospital is aware about these aspects to take into account, from the nurses, doctors, paramedical staff. Everybody understands that. When people arrive at our hospital, nobody will laugh at them. They will smile and be friendly, that is important. We do everything we can so that patient can feel comfortable and proudly say “I am transgender”.
ZSI is the only European manufacturer of artificial urinary sphincters and of malleable and inflatable penile implants, as solutions for male urological problems (incontinence), sexual complications (Erectile Dysfunction), and gender identity procedures (prostheses for trans men and women).